ACEP president Cirillo addresses Virginia ER docs: ‘You can change the world’
Emergency physicians urged to unite, advocate amid mounting pressures at VACEP ‘26
Emergency physicians face mounting pressure from overcrowded hospitals, workforce shortages and powerful insurance companies, but collective action and advocacy remain essential to protecting patient care.
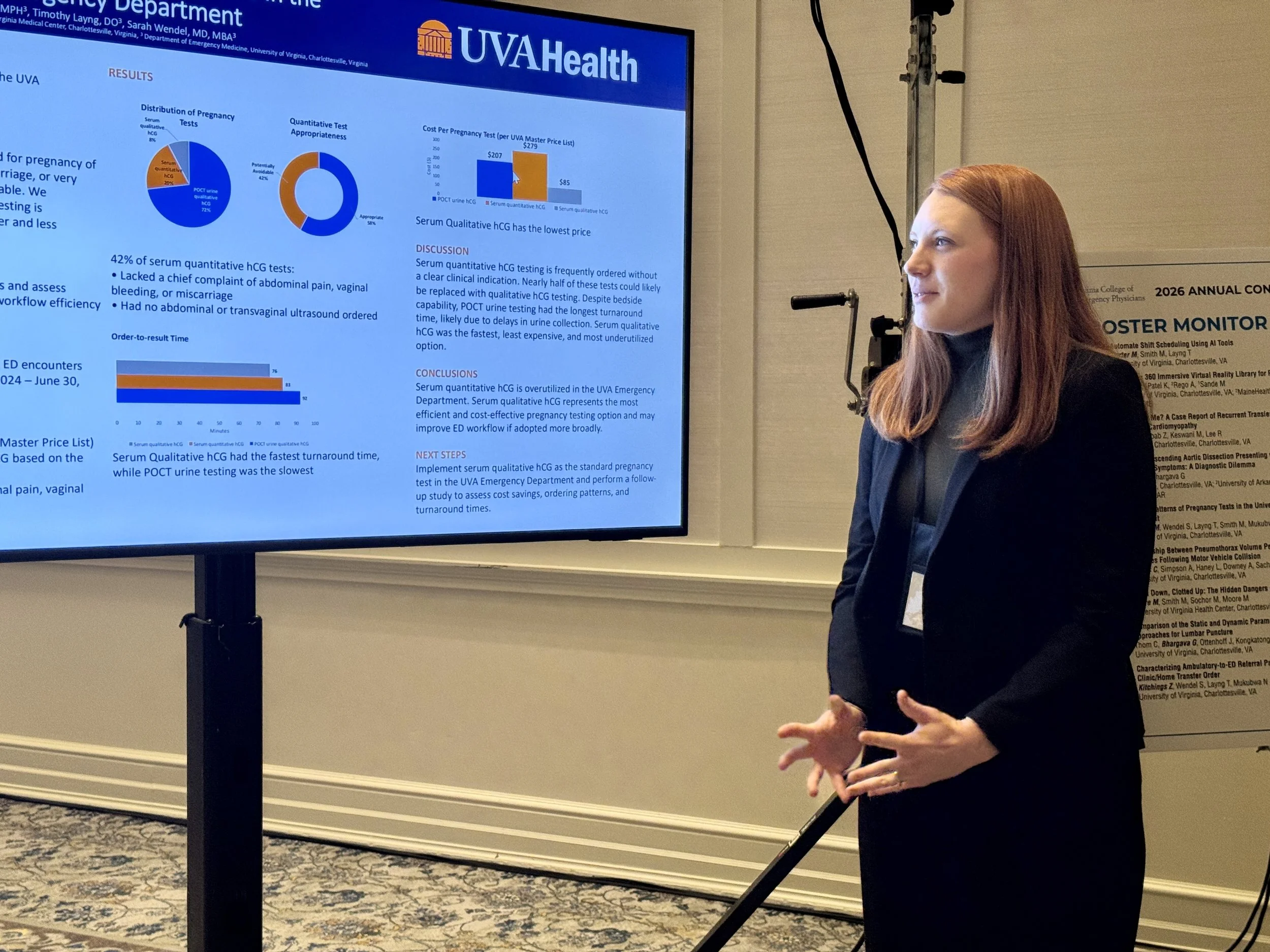
ACEP president L. Anthony Cirillo, MD presented to attendees at the VACEP 2026 Annual Conference in Hot Springs.
That was the message delivered by L. Anthony Cirillo, MD, to attendees of the Virginia College of Emergency Physicians’ annual conference in Hot Springs this month. Cirillo, president of the American College of Emergency Physicians, spoke to attending emergency physicians, residents, and medical students about the challenges confronting emergency medicine and the national organization’s efforts to influence policy and improve working conditions.
Cirillo has practiced emergency medicine for more than 30 years and serves as director of government affairs for US Acute Care Solutions. Since 2022, four ACEP presidents have attended and spoken at the VACEP conference. Cirillo attended last year and returned this year as president.
“You have chosen the hardest of all the specialties,” Cirillo said, describing emergency departments as operating in the “middle of hard” all the time. “That’s a good thing if you turn it into a good thing. But you have to believe that the work we’re doing matters — and it does.”
On the biggest emergency medicine issues
This isn’t new: For years in his presentations, Cirillo has used a 1990 Time magazine cover declaring an “emergency” in American medicine to illustrate how long the field has faced similar challenges.
For years, Cirillo has used a 1990 Time magazine cover declaring an “emergency” in American medicine to illustrate how long the field has faced similar challenges.
He pointed to crowding and boarding, workplace violence and gaps in mental health care as persistent problems. He cited cases in which pediatric patients have waited months in emergency departments for inpatient placement, calling the situation “criminal” and evidence that the system must do better.
He warned that politics and money will always shape health care, noting that high costs and polarized debate complicate reform efforts.
“We are a society that is tearing itself apart,” he said. “We become more and more hyper-polarized and we don’t listen anymore. We just scream louder.”
On HHS leadership
ACEP has approached Robert F. Kennedy Jr.’s oversight of the Department of Health and Human Services through formal engagement, sending letters outlining priorities for emergency medicine and expressing a willingness to collaborate on issues such as crowding, insurer practices and implementation of federal health policy.
At the same time, ACEP has pushed back against Kennedy’s positions, emphasizing the importance of evidence-based public health guidance, including issuing statements urging continued access to vaccines. Other major medical groups have taken more openly critical stances toward Kennedy’s policies.
HHS’s Chris Klomp, whom Cirillo described as nonpartisan and praised an expert who will change how care is paid for in America.
Cirillo highlighted one HHS official he said could make a meaningful difference: Chris Klomp, who built and led care collaboration data network Collective Medical, which years ago worked with Virginia officials to create a system that enables hospitals, EDs, and providers to share patient data, reducing avoidable admissions and enhancing care for high-risk patients.
“Five years ago, nobody would have thought Chris Klomp was going to be in the position that he was in,” Cirillo said. “Now Chris is in a position where he can make significant changes, and he understands emergency medicine. He is apolitical. He doesn’t care about red or blue. What he cares about is data and numbers and efficiency and spending money in a way that makes sense. Chris is going to change how health care is paid for in this country.”
Taking aim at insurers
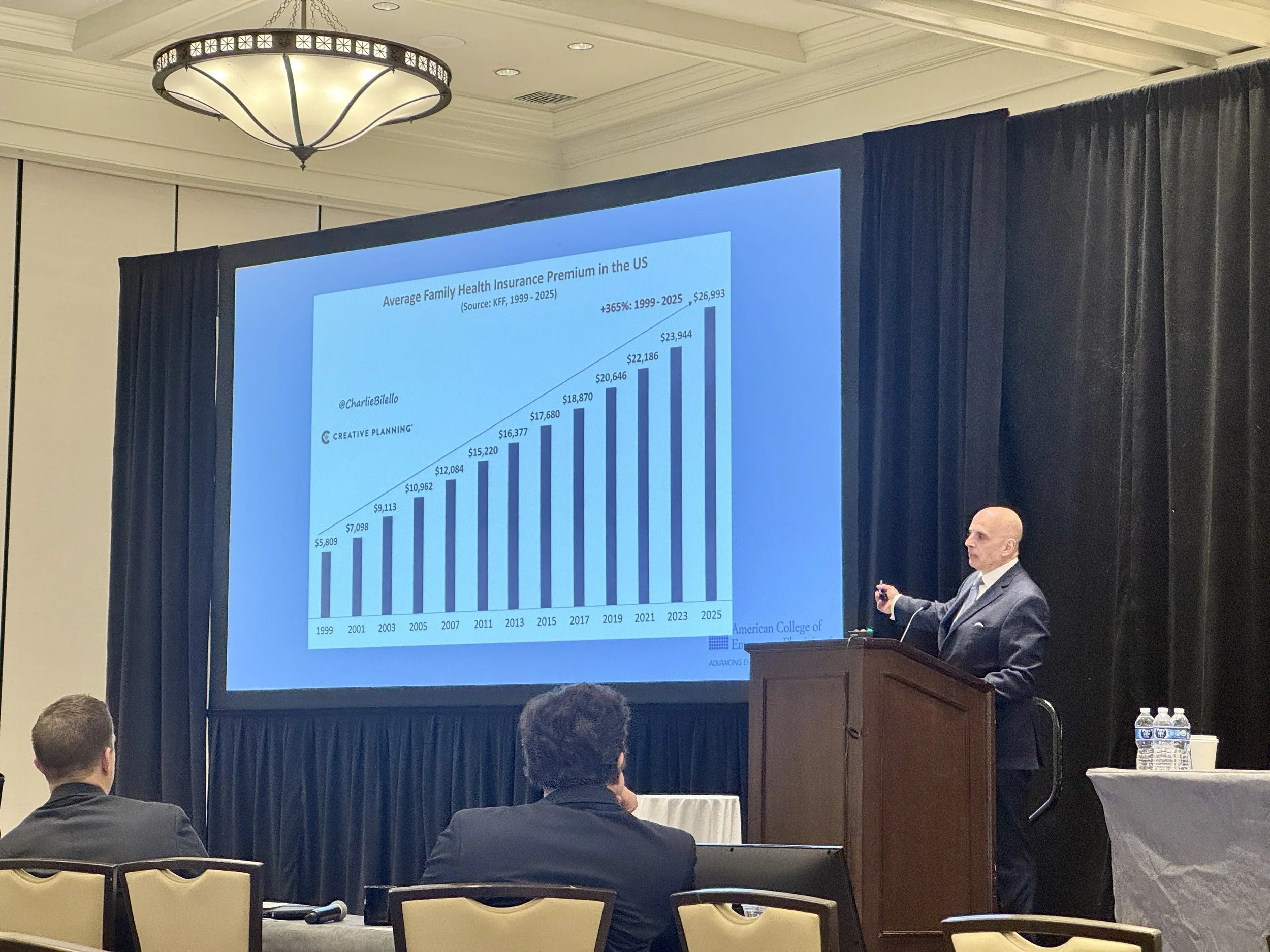
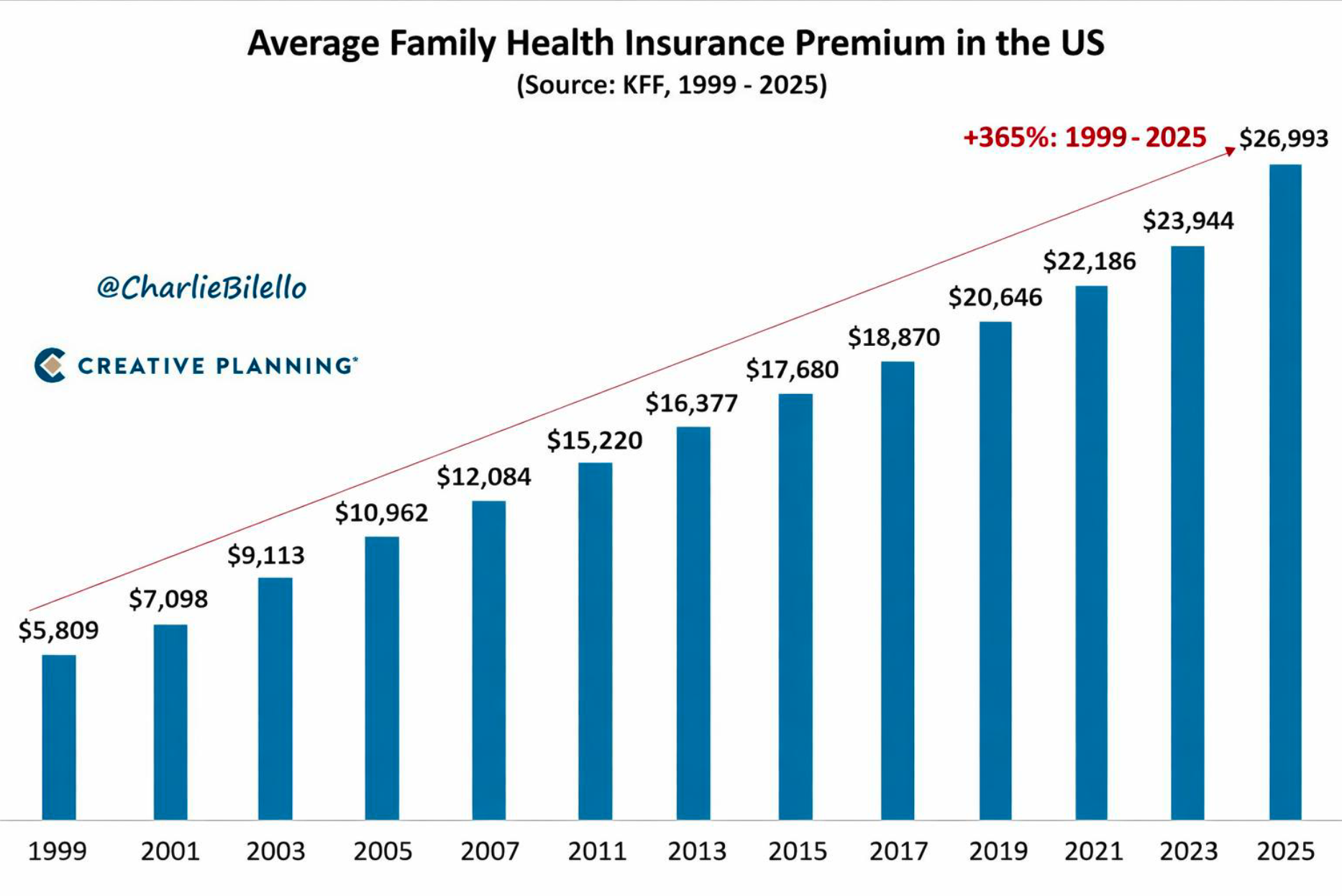
A slide shown in Cirillo’s presentation showing rising health insurance premiums regardless of economic conditions.
Cirillo reserved some of his strongest criticism for health insurers, arguing that consolidation into healthcare systems and profit-driven practices have distorted the marketplace.
“The insurance companies are out of control,” he said.
He said vertically integrated insurers increasingly control payment, pharmacy services and care delivery, limiting options for both patients and physicians.
“They are manipulating the health care market. They are denying care to patients. They are denying you a living wage,” Cirillo said.
Cirillo pointed to steadily rising premiums — regardless of the state of the economy or wage increases — as evidence of systemic dysfunction. “It doesn’t matter if we have a worldwide pandemic,” he said. “Health care premiums go up the same percentage every year. They don't care. That's their job. And anytime they try to tell you anything other than that, they are lying.”
Artificial intelligence and emerging technologies
Cirillo also addressed the growing role of artificial intelligence in health care, calling it a major turning point for medicine while warning against unrealistic expectations.
He emphasized that technology cannot replace clinical judgment or human connection and that data alone is insufficient to drive meaningful reform.
“Any lobbyist can show up with data. But stories convince,” he said, urged physicians to combine data with patient experiences when engaging policymakers, especially as AI tools become more prevalent in clinical and administrative settings. (And you can do so at ACEP’s annual Leadership & Advocacy Conference in April, with visits to Capitol Hill).
On Virginia’s ACEP chapter
Cirillo praised Virginia’s ACEP leaders, saying they have “prosecuted and passed legislation that has changed the practice and how we take care of patients probably better than any other ACEP chapter.”
Enduring challenges in emergency medicine
Throughout his animated and at times humorous talk, Cirillo outlined longstanding problems facing emergency departments, including crowding, workplace violence and inadequate mental health resources.
He said addressing these challenges requires professional unity and clarity about the role of emergency physicians. “At some point you have to stand up and say who we are and how we train makes us different,” he said.
He noted that ACEP recently strengthened its ED staffing policy: That all emergency departments should be staffed by an emergency physician.
Despite the difficulties facing U.S. emergency departments, Cirillo said he finds some reassurance in international comparisons, noting that physicians in other developed countries face many of the same challenges.
ACEP advocacy beyond the talking points
Cirillo’s remarks echoed broader efforts by ACEP to influence federal and state policymakers, protect physician autonomy and improve conditions for patients and providers alike. The organization maintains a dedicated advocacy presence in Washington and at the state level, engages members in grassroots action and drives legislative and regulatory change affecting emergency care.
He highlighted ACEP’s accreditation program as a key effort to improve safety and quality in emergency departments — and as a way to secure additional resources from hospital leadership.
“Many CEOs like to hang banners out in front of their hospital,” Cirillo said, explaining that accreditation allows emergency departments to gain visible recognition and use the idea of gaining accredited status as leverage for staffing and support.
He also discussed recent policy battles, including ACEP’s recent decision to withdraw support from international sepsis guidelines that lacked meaningful emergency physician leadership and its call for greater transparency from the Accreditation Council for Graduate Medical Education on residency standards.
Key ACEP advocacy priorities include:
Federal and state legislative engagement, including work on the No Surprises Act, ED crowding and reimbursement.
Physician-led care campaigns promoting emergency physician leadership.
Regulatory advocacy involving Medicare, Medicaid and federal rulemaking.
Grassroots mobilization through the 911 Grassroots Network and the Leadership & Advocacy Conference
Guidance for residents and young physicians
Much of Cirillo’s message was directed at residents and medical students in the room, whom he encouraged to become involved in advocacy and professional leadership early in their careersHe urged young physicians to engage directly with lawmakers, noting that many congressional staffers shaping health care policy are young and inexperienced.
Cirillo emphasized that progress depends on collaboration within the specialty and across health care.“We are the family of people who have chosen the hardest profession. We are here to make a difference in the world.”
He closed by reflecting on what he called the “restorative moment” in emergency medicine — the instant when a patient places their life in a physician’s hands. “This moment, when another human being who doesn't know you, literally trusts their life into your hands…I promise you, who you are in that moment changes that person’s life. In that moment, you can change the world.”
PHOTO GALLERY: VACEP 2026 ANNUAL CONFERENCE
FEB 20-22, 2026, HOT SPRINGS, VIRGINIA